Note: If you're more of a visual learner, watch a video on this topic.
At times, carriers will request evidence of insurability (EOI) for voluntary benefits when the plan participant chooses a coverage amount that is over the guaranteed issue amount (the amount that is pre-approved by the carrier). The carrier will also require EOI if the plan participant is a late entrant. This article covers how to approve or deny the total requested amount in Maxwell once you hear back from the carrier on their EOI decision.
How to approve or deny the total requested amount
 |
Please Note: You do not need to take this step for Sun Life benefits as the decision will be processed on your behalf! Learn more > |
- Head to the enrolled benefit on the employee's profile and click Process EOI Request >>
- Check the box to approve or deny coverage for the employee.
- If you approve the employee and there’s dependent coverage pending that you’re still waiting for a decision on, you can select “Process at a later date” for the dependent. This will keep the dependent coverage pending.
- If you’re approving coverage, add an effective date.
- If you want to send an email to the employee notifying them that this has been processed, check the box “Notify employee of processed request.”
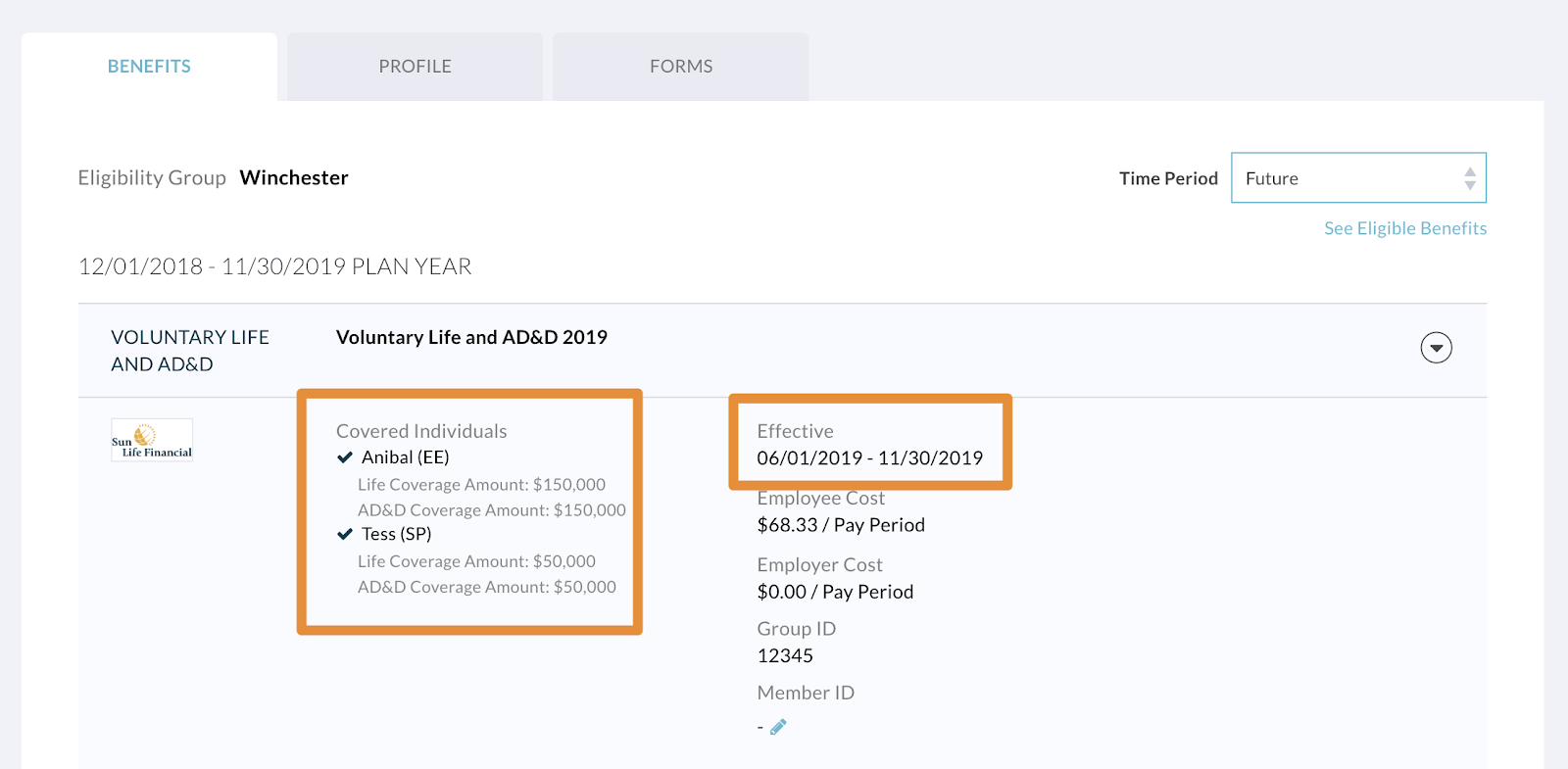
- Head to the “Benefits” tab and notice that approved amounts will display (as of the new effective date that you entered) on a new enrollment for the same voluntary plan.