COBRA is a provision that requires continuation of coverage to be offered to covered employees, their spouses, former spouses, and dependent children when group health coverage would otherwise be lost due to specific “qualifying” events.
Many employers hire a COBRA administrator to help them fulfill COBRA requirements including providing notices and having individuals elect continuation of coverage. Maxwell does not act as a COBRA administrator. But you will use Maxwell to manage qualifying events that cause an employee to be eligible for COBRA coverage.
Maxwell has integrations with leading COBRA administrators Discovery Benefits and Accrue Solutions, as well as the ability to connect with any COBRA vendor that can accept our standard EDI file. If you are a Discovery or Accrue COBRA client and would like more information on setting up the integration, or are interested in setting up a connection with your COBRA vendor, reach out to your Advisor. You can also learn more about the integrations here.
NOTE: To learn more about COBRA, the requirements under the law, or whether or not a specific employee is eligible for COBRA, we recommend consulting with your benefits advisor, your COBRA administrator, and/or online resources like the U.S. Department of Labor’s website here.
In this article:
- COBRA Terminology
- Run an Initial COBRA Rights Report
- Marking COBRA Eligibility Due to a COBRA Qualifying Event
- Run a COBRA Qualifying Event Report
- Notes
Before jumping into the steps to marking COBRA eligibility, let’s talk COBRA terminology.
COBRA Qualifying Events
These are the events that make employees, and/or their spouses and children eligible for COBRA. Below is a list of those events, who is typically eligible, and how that event translates to the Change Reason in Maxwell.
| Name of COBRA Qualifying Event in Maxwell | Full Description | Who is Typically Covered | Related Change Reasons in Maxwell |
| Termination | Termination of the employee's employment for any reason other than gross misconduct | Any individuals covered on the plan (employee, spouse, dependents) at the time of the event |
Termination (learn how to terminate an employee here) |
| Reduction of Hours | Reduction in the number of hours of employment | Any individuals covered on the plan (employee, spouse, and dependent children) at the time of the event | Employee Lost Eligibility |
| Entitled to Medicare | Covered employee becomes entitled to Medicare | Spouse and dependent children covered on the plan at the time event | Employee Newly Eligible for Medicare |
| Divorce or Legal Separation | Divorce or legal separation of the spouse from the covered employee | Spouse and dependent children covered on the plan at the time of the event | Divorce or Legal Separation |
| Death | Death of the covered employee | Spouse and dependent children covered on the plan at the time of the event |
Termination with Termination Reason of “Deceased Employee” |
| Dependent Age Off | Loss of dependent child status under the plan rules | Dependent child covered on the plan at the time of the event | Dependent Age Off |
COBRA Qualifying Event Date
This is the date that the COBRA Qualifying Event occurred. As an example, if the COBRA Qualifying Event is Termination, then the COBRA Qualifying Event Date would be the date of the Termination.
COBRA Eligibility Date
This is the date the employee or dependents are eligible to begin COBRA coverage, should they choose to enroll in it. This date will always be after the COBRA Qualifying Event Date or product end date, as COBRA coverage usually kicks in the day after active coverage ends.
COBRA Eligible Individuals
These are all individuals eligible for COBRA coverage due to the COBRA Qualifying Event. The eligible individuals will always be assumed to be the individuals who are covered on the product, unless the COBRA Qualifying Event is Dependent Age Off or Divorce or Legal Separation. In these cases, you can customize which individual(s) are eligible for COBRA. They will be marked eligible for any of the COBRA-eligible products they’re actively covered on.
Run an Initial COBRA Rights Report
Run a report to pull an .xls file listing all individuals (employees and dependents) who became newly enrolled in a coverage that may qualify for a COBRA rights notice based on a specific time period. This is helpful whether you’re looking to send the file right over to a COBRA administrator, or managing sending the notice yourself. Follow the steps below:
- Head to Tools > Reports > Library and click into the “Initial COBRA Rights Report.”
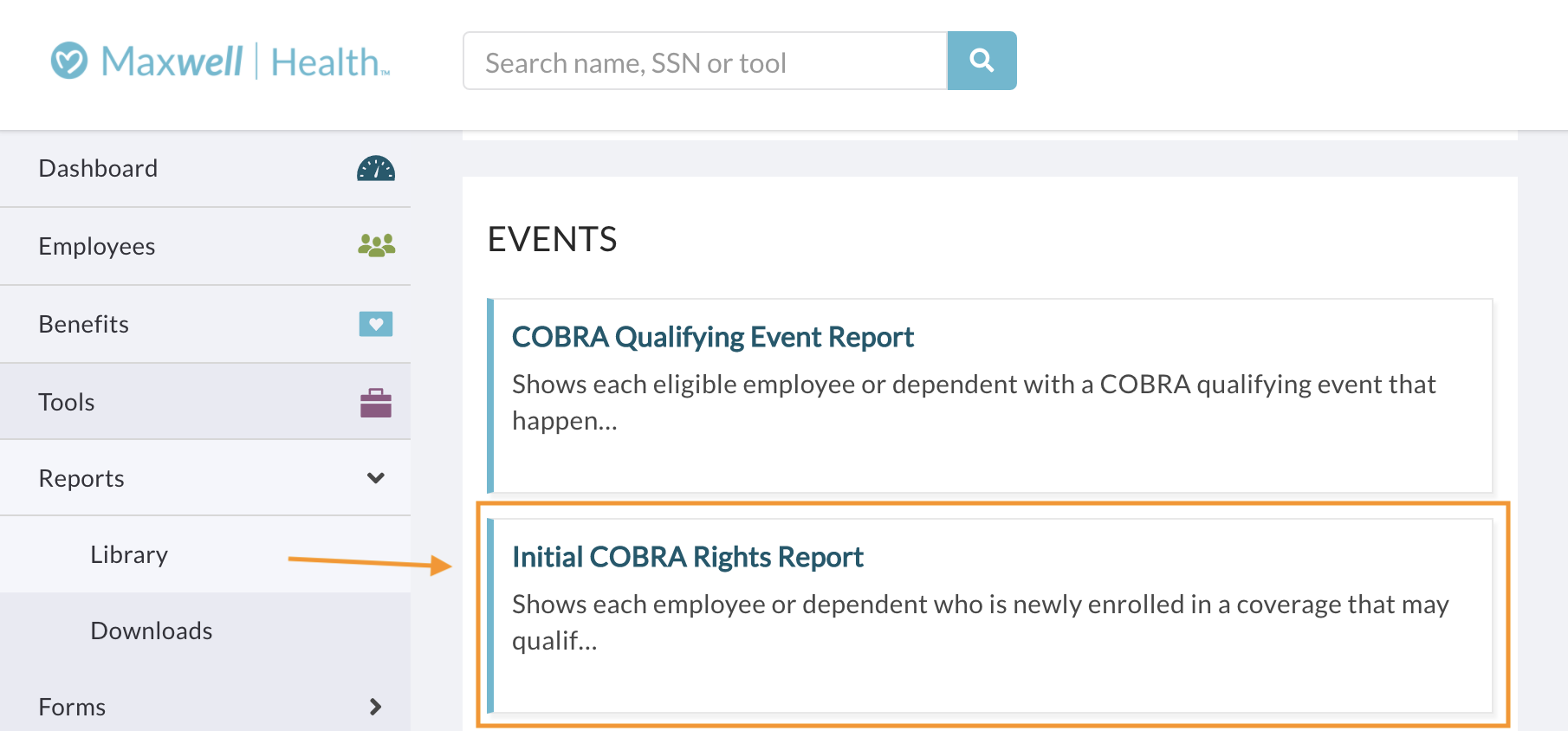
- Customize the report with the information you’d like to see
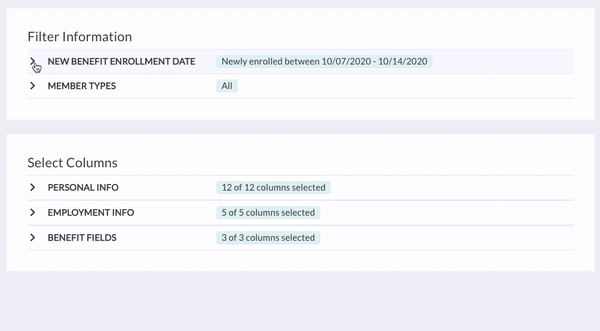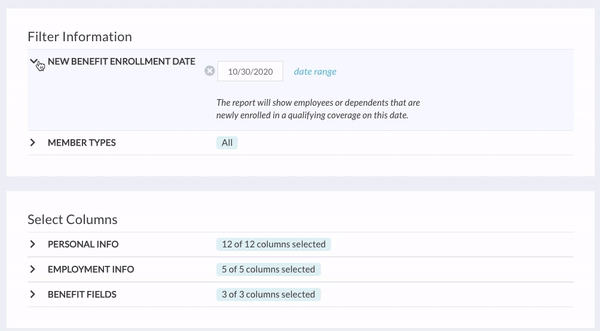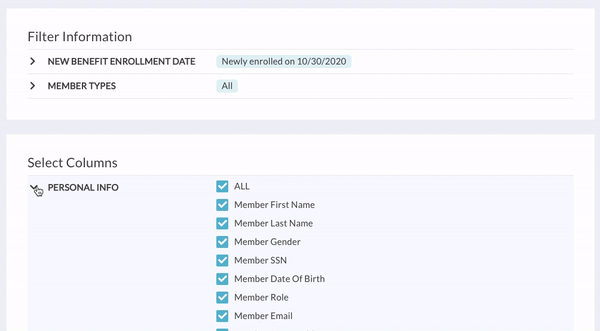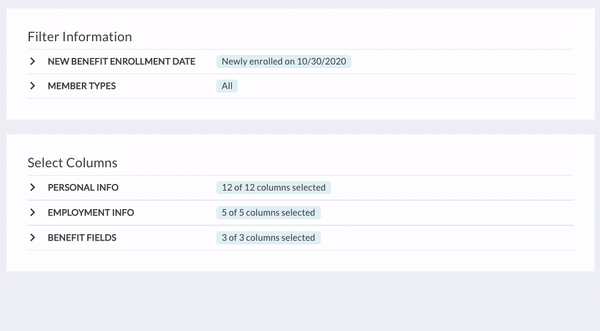
- The New Benefit Enrollment Date filter will already be set to pull information on individuals who newly enrolled in coverage for a one-week period starting today. You can adjust this to a different date range or single date to get what you’re looking for.
- You can also remove columns, depending on the information you or your COBRA administrator needs. If you’d like, save the report as a custom report to come back to in the future.
- When you’re done, click Generate Report. You can download the report from your "Recently Generated Reports" section.
Marking COBRA Eligibility Due to a COBRA Qualifying Event
Follow these steps to mark an employee COBRA-eligible due to a qualifying event:
- Step One: Indicate a coverage change in Maxwell. How you’ll do this depends on the type of COBRA Qualifying Event.
- For Terminations and Death of a covered employee, you will first terminate the employee by clicking Options > Terminate Employee on the employee’s profile
- After you fill out the relevant dates and termination reason and click Terminate Employee, click Terminate & Continue to COBRA to complete the termination and continue to COBRA eligibility.
- After you fill out the relevant dates and termination reason and click Terminate Employee, click Terminate & Continue to COBRA to complete the termination and continue to COBRA eligibility.
- For Reduction of Hours, Entitled to Medicare, Divorce or Legal Separation, and Dependent Age Off qualifying events, you’ll first change the employee’s coverage and/or information based on the corresponding change reasons listed in the table above. Once you’ve ended the change event and processed product changes, click Options > Manage COBRA Event.
- Step Two: Once you’re on the COBRA eligibility screen, complete the following fields:
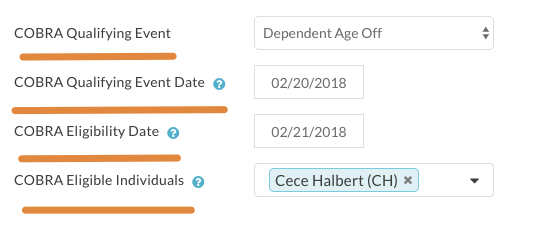
- COBRA Qualifying Event. If you went through the termination workflow, this field is pre-populated to “Termination.” You’ll want to change this to “Death” in the rare scenario where the termination reason was “decreased employee.”
- COBRA Qualifying Event Date. Note: If you went through the termination workflow, this field will be pre-populated to reflect the Date of Termination.
- COBRA Eligibility Date. Note: If you went through the termination workflow, this field will be pre-populated to the day after the Date of Product Termination (i.e. - not the day after the employee is terminated, but the day after the benefits coverage ends).
- COBRA Eligible Individuals. Note: This field will only exist for Dependent Age Off and Divorce or Legal Separation.
- Step Three: Review the products listed as eligible for COBRA, and adjust the COBRA eligibility for any as necessary. Please note that the system pulls all medical, dental, vision, and financial products the employee is or was recently enrolled in. While these products typically offer continuation of coverage under COBRA, you may want to double check your plan design/summary document to make sure that’s the case. Note that if a dependent is aging off a particular product, you’ll definitely want to make sure you toggle COBRA eligibility off for all other products, as they do not relate to this event.
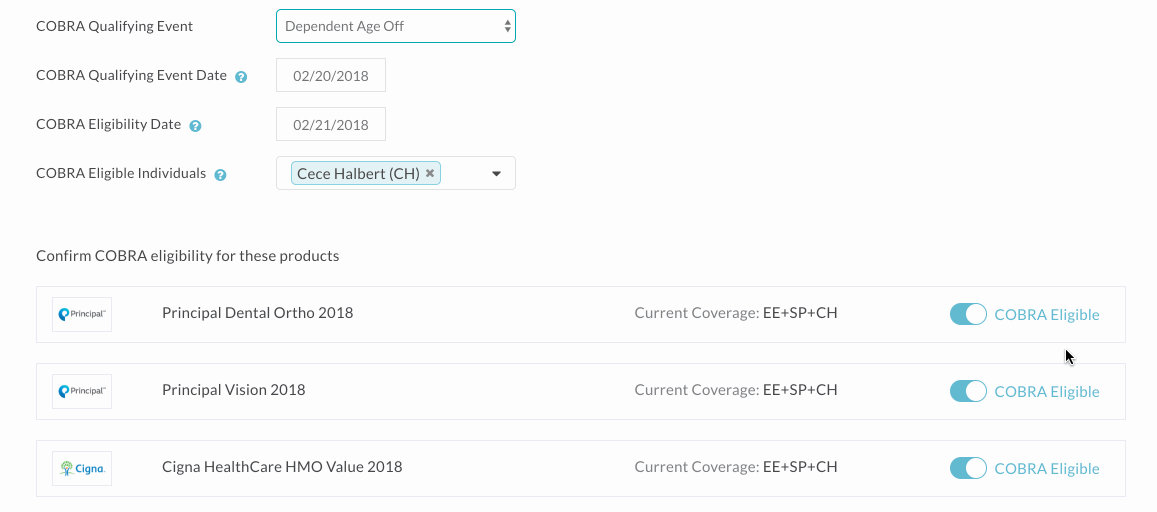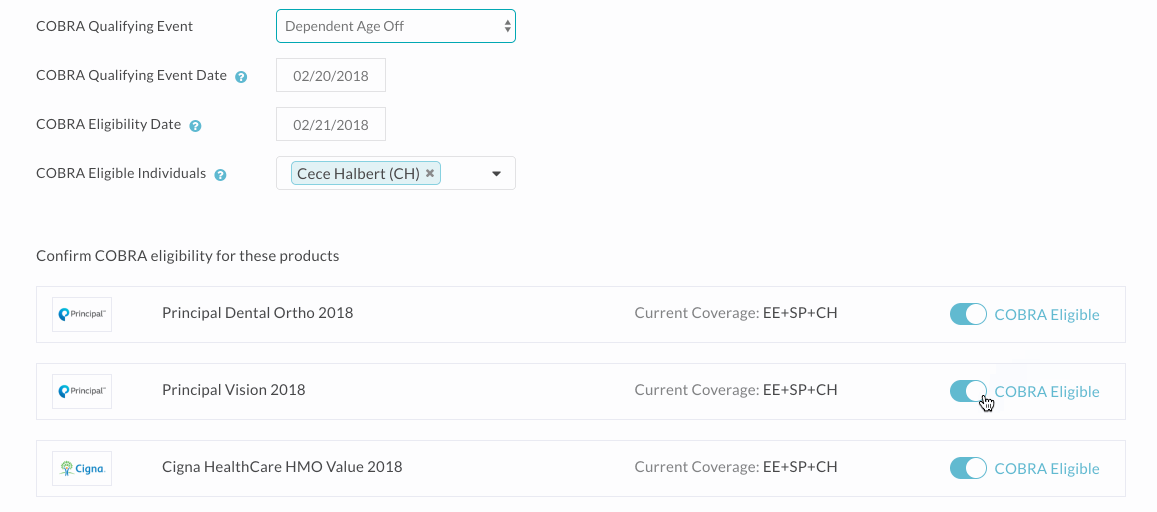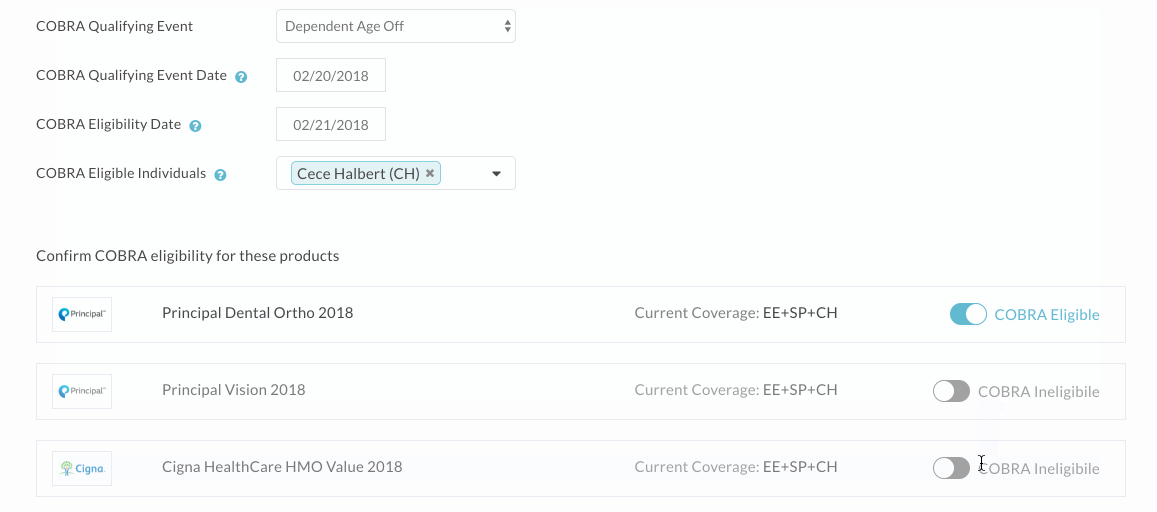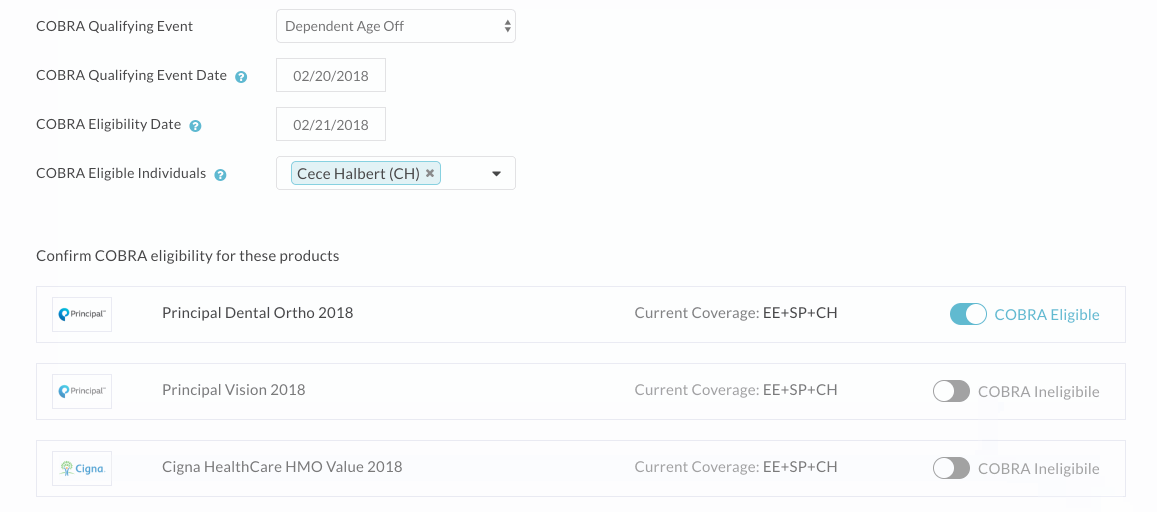
- Step Four: When you’re all set, click Confirm COBRA eligibility and OK to mark the employee COBRA-eligible. Their employee profile will display their COBRA Eligibility Date, even in the case where it’s a dependent who is eligible for COBRA coverage.
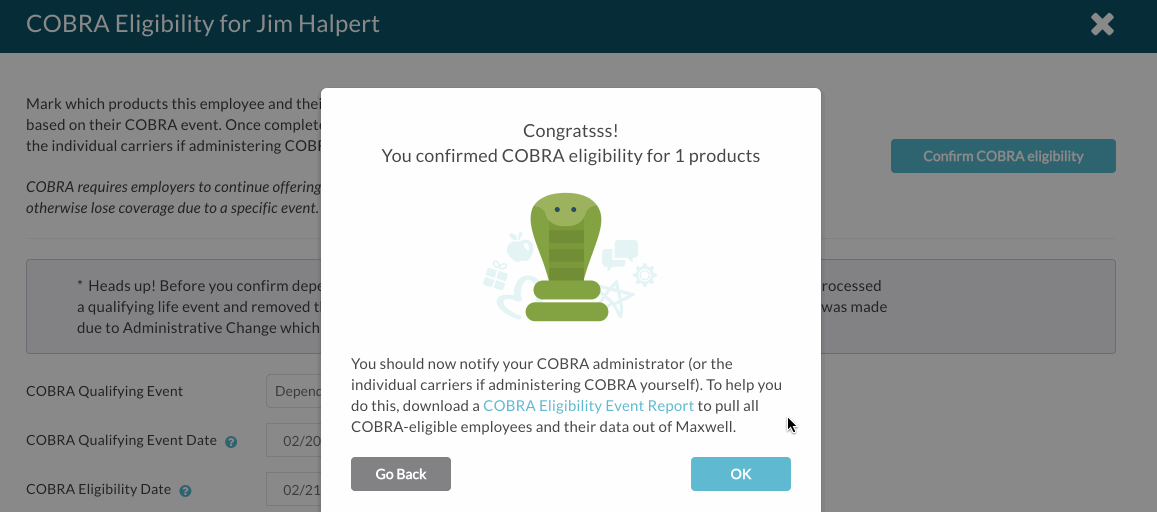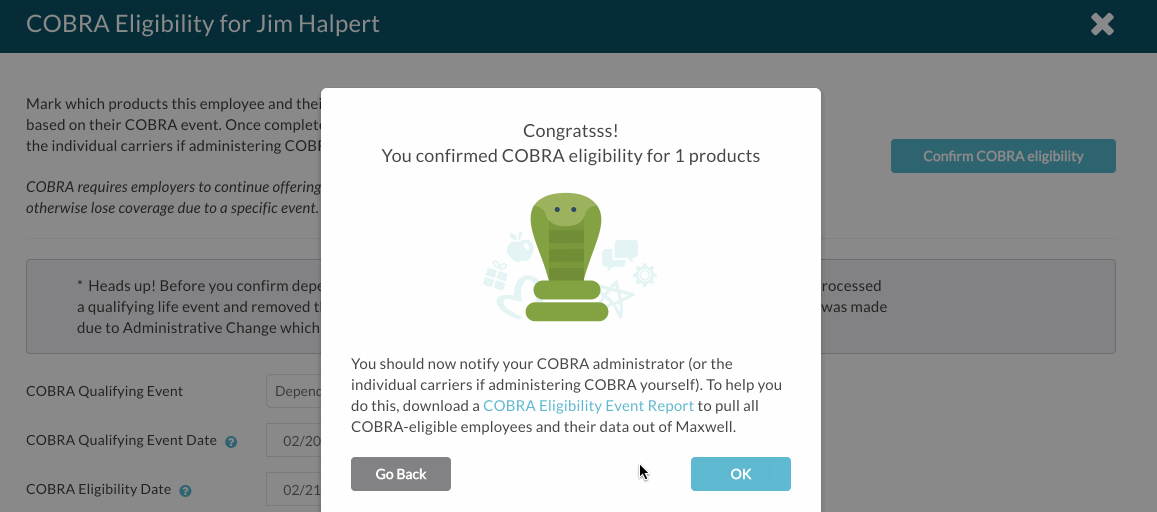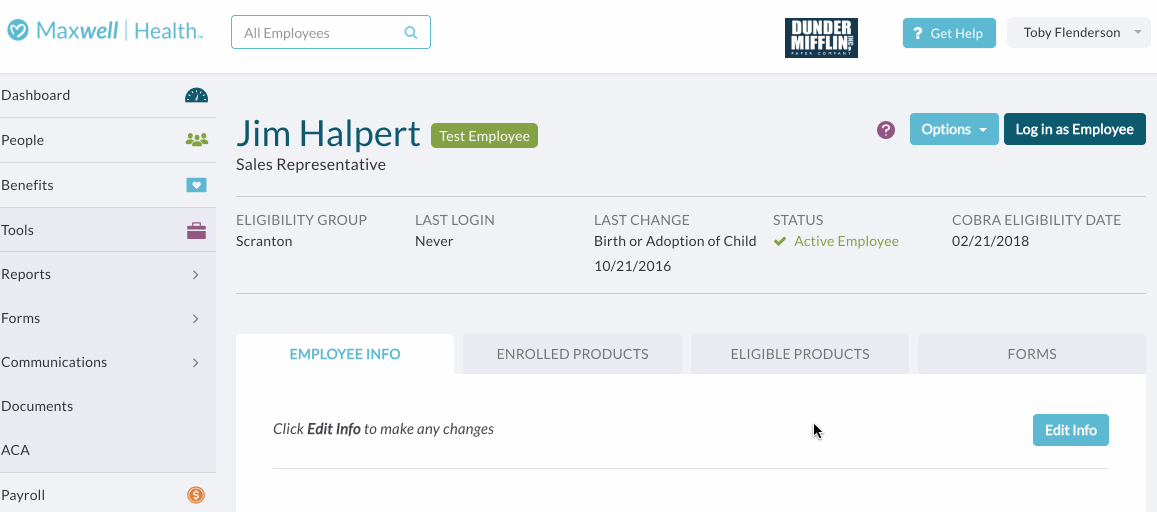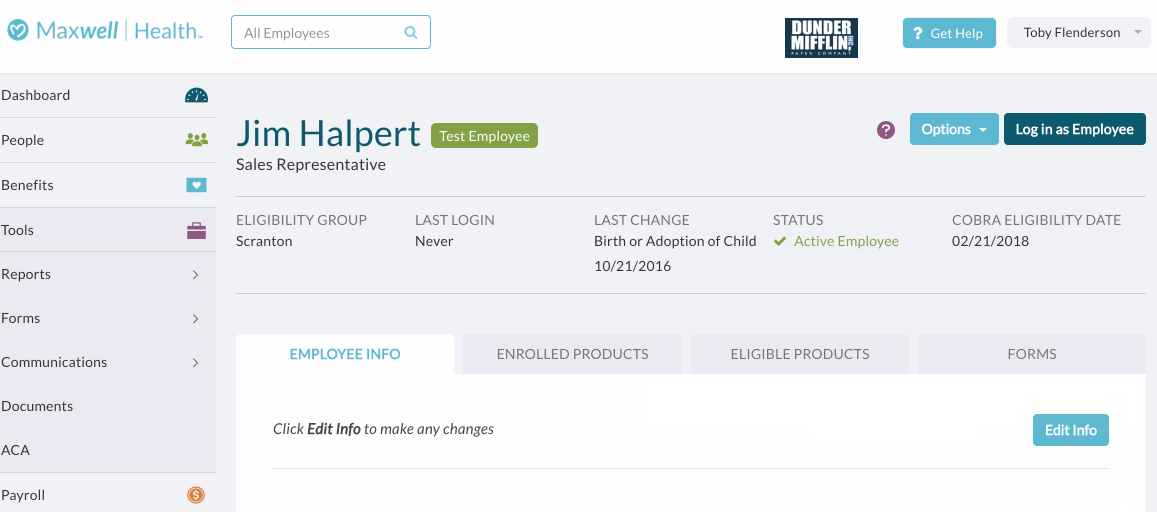
See below for instructions on how to see a report with all COBRA eligibility information. If you're using a COBRA integration, this information will be sent to the administrator on the next file (which runs every Monday morning at 5am ET).
Run a COBRA Qualifying Event Report
Run a report to pull an .xls file listing all individuals (employees and dependents) who became COBRA-eligible during a defined period of time. This is helpful whether you’re looking to send the file right over to a COBRA administrator, or get the information over to the carriers yourself. Follow the steps below:
- Head to Tools > Reports > Library and click into the “COBRA Qualifying Event Report.”
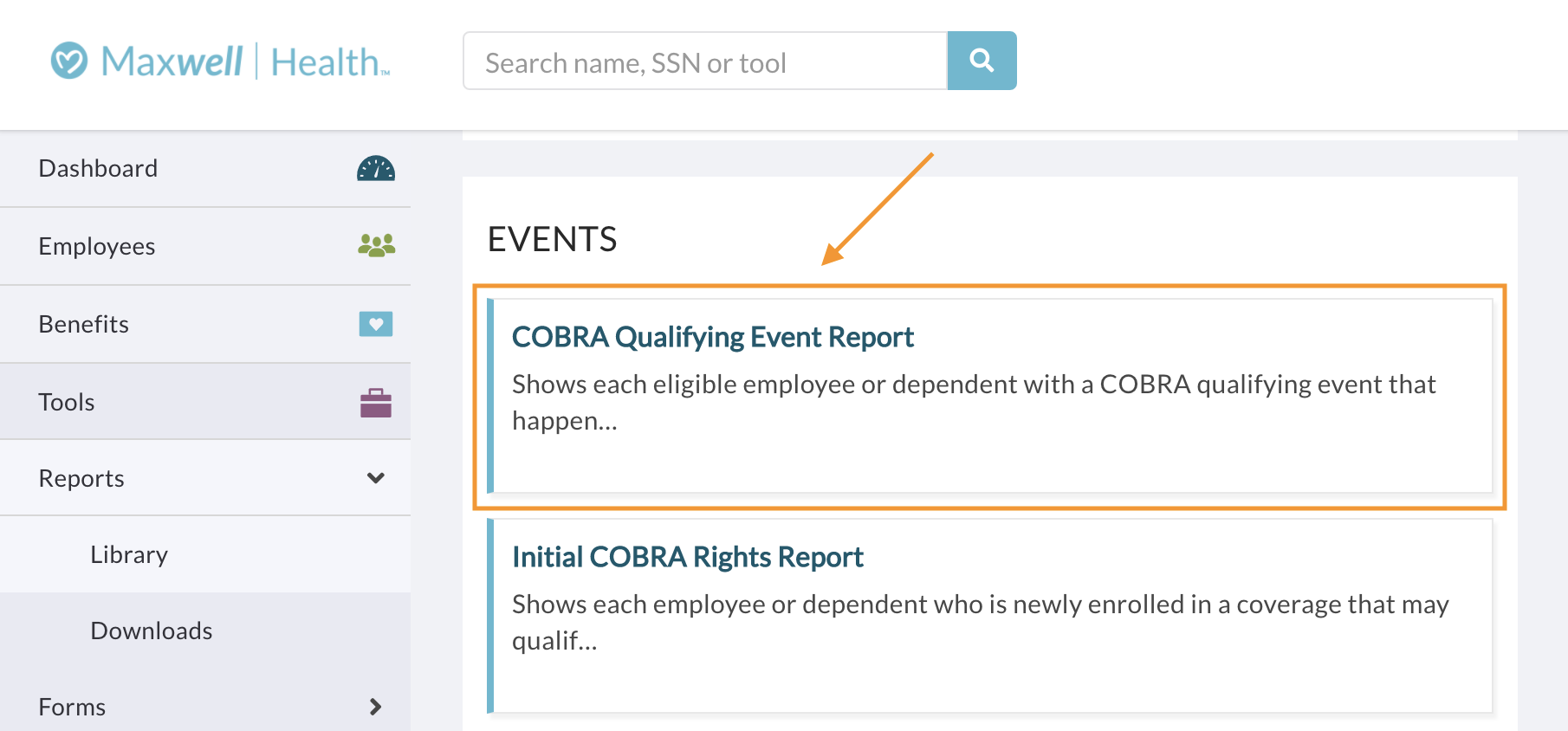
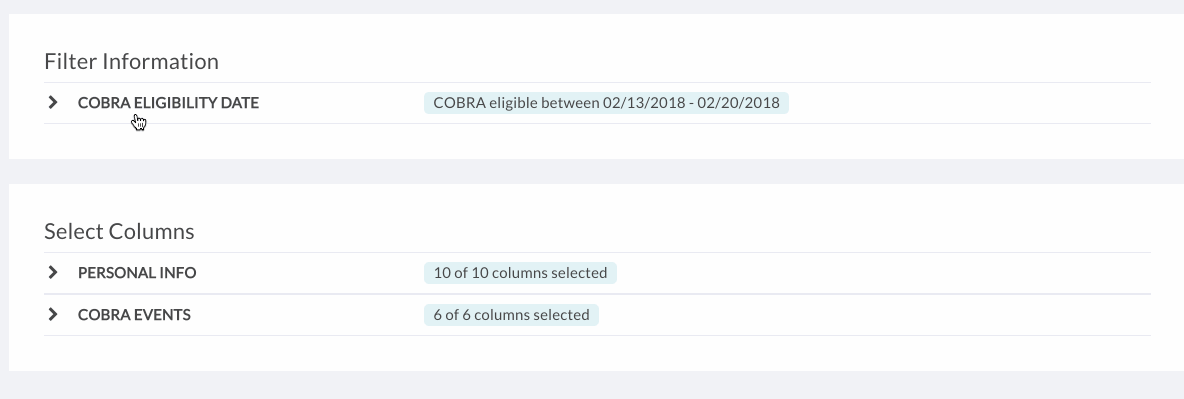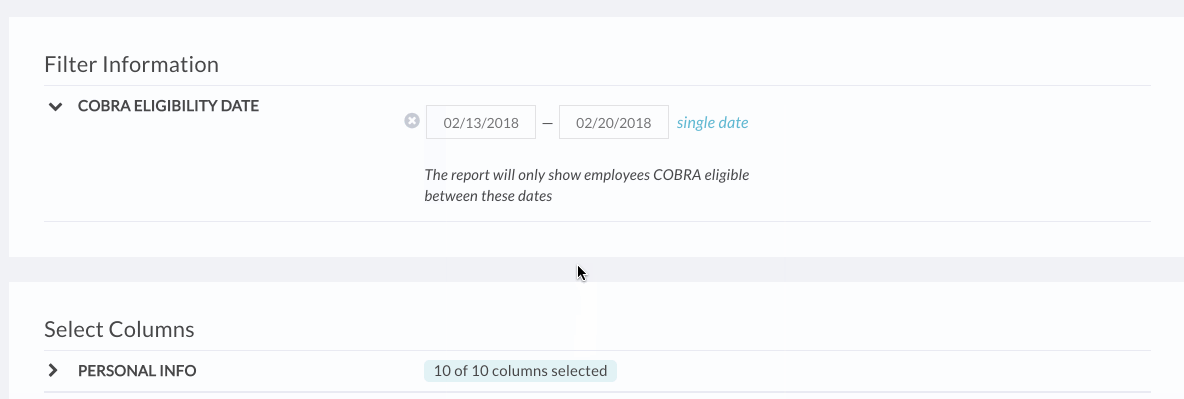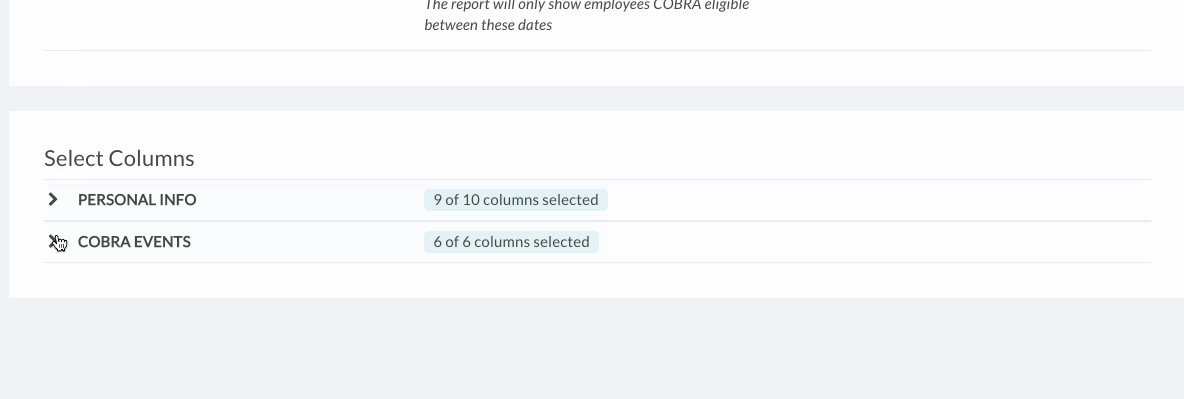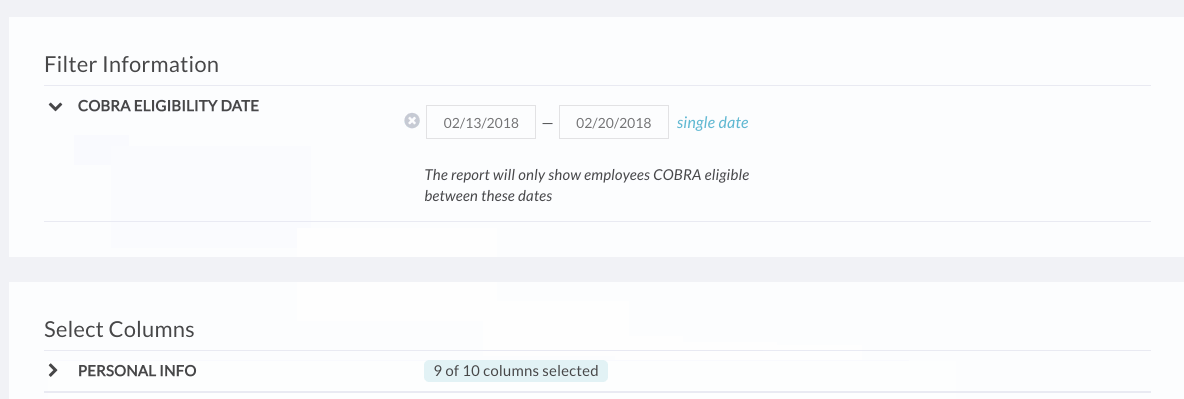
- Customize the report with the information you’d like to see
- The COBRA Eligibility Date filter will already be set to pull information on individuals who became COBRA eligible over the past week. You can adjust this to a different date range or single date to get what you’re looking for.
- You can also remove columns, depending on the information you or your COBRA administrator needs. If you’d like, save the report as a custom report to come back to in the future.
- When you’re done, click Generate Report. You can download the report from your "Recently Generated Reports" section.
- Maxwell does not act as the COBRA administrator. Among other things, this means that employees will not log into Maxwell Health to make their COBRA elections.
- Maxwell does not track the entire time period during which the individual is eligible for COBRA coverage, only when they became COBRA-eligible due to a qualifying event.
- If you marked an individual COBRA-eligible on accident, please reach out to Customer Support at support@maxwellhealth.com to reverse that change.
- You can mark products as COBRA-eligible within 45 days of them being terminated. This is because COBRA requires that the employer provide notice of a COBRA qualifying event such as termination to the plan administrator within 30 days.